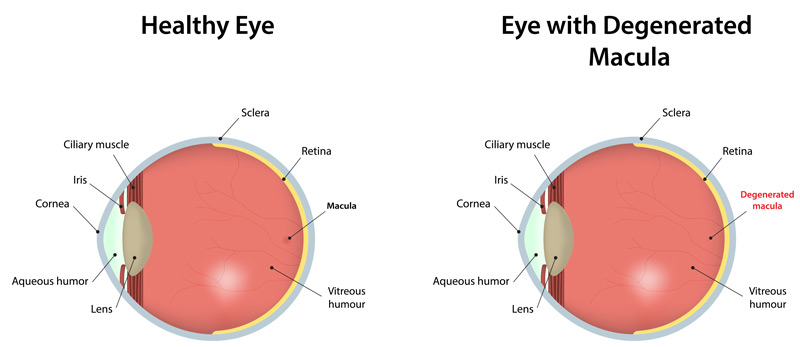
Macular degeneration is damage or breakdown of the macula of the eye. The macula is a small area at the back of the eye that allows us to see fine details clearly. When the macula doesn’t function correctly, we experience blurriness or darkness in the center of our vision. Macular degeneration affects both distance and close vision and can make some activities like threading a needle or reading difficult or impossible. Although macular degeneration reduces vision in the central part of the retina, it does not affect the eye’s side, or peripheral, vision. For example, you could see the outline of a clock but not be able to tell what time it is. Macular degeneration alone does not result in total blindness. People continue to have some useful vision and are able to take care of themselves.
What Causes Macular Degeneration?
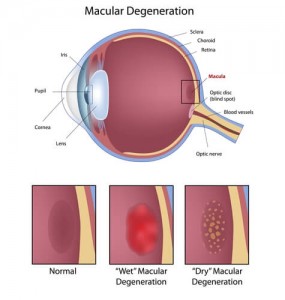
Many older people develop macular degeneration as part of the body’s natural aging process. The two most common types of age-related macular degeneration are “dry” (atrophic) and “wet” (exudative):
“Dry” Macular Degeneration (Atrophic)
Most people have “dry” macular degeneration. It is caused by aging and thinning of the tissues of the macula. Vision loss is usually gradual.
“Wet” Macular Degeneration (Exudative)
“Wet” macular degeneration accounts for about 10% of all cases. It results when abnormal blood vessels form at the back of the eye. These new blood vessels leak fluid or blood and blur central vision. Vision loss may be rapid and severe.
What are the Symptoms of Macular Degeneration?
Macular degeneration can cause different symptoms in different people. The condition may be hardly noticeable in its early stages. Sometimes only one eye loses vision while the other eye continues to see well for many years.
But when both eyes are affected, the loss of central vision may be noticed more quickly. Following are some common ways vision loss is detected:
- Words on a page look blurred.
- A dark or empty area appears in the center of vision.
How is Macular Degeneration Diagnosed?
Many people do not realize that they have a macular problem until blurred vision becomes obvious. Your ophthalmologist (medical eye doctor) can detect early stages of macular degeneration during a medical eye examination that includes the following:
- Viewing the macula with an ophthalmoscope.
- A simple vision test in which you look at a grid resembling graph paper.
- Sometimes special photographs, called angiograms, are taken to find abnormal blood vessels under the retina.
- Fluorescent dye is injected into your arm and your eye is photographed as the dye passes through the blood vessels in the back of the eye.
How is Macular Degeneration Treated?
Despite ongoing medical research, there is no cure yet for “dry” macular degeneration. Some doctors believe that nutritional supplements may slow macular degeneration, although this has not yet been proven. Treatment of this condition focuses on helping a person find ways to cope with visual impairment.
In its early stages, “wet” macular degeneration can be treated with laser surgery, a brief and usually painless outpatient procedure. Laser surgery uses a highly focused beam of light to seal the leaking blood vessels that damage the macula. Although a small, permanently dark “blind spot” is left at the point of laser contact, the procedure can preserve more sight overall.
Despite advanced medical treatment, people with macular degeneration still experience some vision loss.
Your ophthalmologist can prescribe optical devices or refer you to a low vision specialist or center. A wide range of support services and rehabilitation programs are also available to help people with macular degeneration maintain a satisfying lifestyle.
Because side vision is usually not affected, a person’s remaining sight can be very useful. Often, people can continue with many of their favorite activities by using low vision optical devices such as magnifying devices, closed-circuit television, large-print reading materials, and talking or computerized devices.


